Healing means acting, it is not a passive event.
– Caroline Myss –
Ankle Arthritis
Ankle arthritis is a chronic disease that affects the joints (arthropathy).
It can affect all the joints, from the spine to the upper and lower limbs.
It is a degenerative disease, caused by the progressive loss of the cartilaginous tissue, which normally covers the joint, exposing the underlying bone (sub-chondral bone) and determine a progressive alteration of the morphology of the joint.
Therefore, it is not a disease of cartilage alone, but of the entire joint:
- skeletal structures;
- ligaments;
- capsular structures,
and even the muscles, connected with joint movement, are involved.
Speaking specifically of the ankle, Dr. Steven Raikin (orthopedic of the Rothman Institute in Philadelphia and member of the AFAS) has recently shown that ankle arthritis has an extremely negative impact on the quality of life of those affected, with equal consequences to that generated from hip osteoarthritis and even worse than that of knee osteoarthritis.
In general, the prevalence of arthritis is directly related to age. However, in the case of ankle arthritis, this evidence is not valid.
In fact, the ankle, unlike the knee and the hip, is a joint that us doctors call extremely congruent because one joint surface corresponds exactly to the other.
If, on one hand, it represents a protective factor against degenerative arthritis, on the other hand it explains how a traumatic event, able to alter the anatomy of the ankle, is sufficient to cause serious arthritic alterations.
This is why around 70% of ankle arthritis has a post-traumatic origin.
Patients who have reported malleolar, tibia, fibula, talus or calcaneal fractures, even if healed (more or less well), are candidates for developing ankle arthritis.
To this, we add patients suffering from ankle instability due to ligament injuries or deformities.
In the remaining situations ankle arthritis is caused by chronic inflammatory systemic diseases, such as rheumatoid arthritis, or other pathologies capable of inducing joint alterations, such as hemophilia.
TopNext
Ankle Arthritis Symptoms
The main symptom of ankle osteoarthritis is pain associated with stiffness.
At the beginning of its manifestation, the pain becomes more acute after long hours of immobility, such as after waking up in the morning. With the resumption of movement during the day these symptoms diminish, even if they may present moments of exacerbation.
In later phases of the disease, however, the pain also appears at rest. It is deep and not very localized due to previous joint overload or meteorological changes.
The joint may appear swollen, stiff, painful to palpation, passive movements and, of course, to ambulation.
Moreover, during movement, crackles or rattles may be felt due to the incongruity of the articular heads and / or the presence of osteophytes.
Finally, because of its preponderant post-traumatic nature – in 70% of cases, as mentioned above – the ankle can be deformed and misaligned.
This is because the reduction and synthesis surgeries, performed after an ankle fracture, do not always manage to restore the correct anatomy of the joint.
TopNext
Diagnosis
Once the disease has been diagnosed and followed by an adequate assessment of the symptoms, it will be necessary to proceed with appropriate assessment tests.
An X-ray is sufficient to highlight the characteristic signs of osteoarthritis:
- thinning of the articular line;
- remodeling of the subchondral bone;
- formation of osteophytes (small bone spurs);
- geodes (osseous cysts).
In the case of an operation being necessary more detailed clinical exams are recommended.
Since the ankle functions in the feet, it is here that it will have to return to function. Therefore, foot and ankle X-rays are necessary to study the alignment and the surgeries necessary to obtain a stable implant over time.
For this reason, I would like to point out that, although there is contrary opinion, the MRI does not provide more advanced information than X-rays. This is because it is performed when lying down and therefore without any pressure on the foot, which is a very important factor for assessing the functionality of the ankle.
In addition to what is recommended above, I think it is important to perform an X-ray projection, conceived by my colleague Donald I. Saltzman, which is performed with the foot inclined at 20 degrees.
It is a simple X-ray performed in a position that allows a better study of the correlation between the position of the calcaneus, of the talus (talus), and of the tibia.
Finally, to study the quality of the bone to be treated, an ankle and a back-to-back CT scan are equally important in planning.
TopNext
How do you Cure Ankle Arthritis?
Ankle osteoarthritis is an irreversible degenerative disease. This means that you can try to control it, but the recovery of a damaged joint is not yet an available result.
NSAIDs (Non-Steroidal Anti-inflammatory drugs) are useful for pain control, but their prolonged use is not advisable due to possible side effects (gastritis and ulcers).
The use of opioids, such as morphine, is also not recommended because it can lead to addiction and cortisone, which is associated with osteoporotic and infectious risk.
To summarize, the pharmacological approach can help in certain phases of the patient’s life, but it does not represent the long-term solution.
There are physical therapies, such as Interx and Tecar Therapy, which are even more effective if performed together. These therapies improve the biology and function of the tendons and muscles used for joint movement. These can represent, in the initial stages of arthritis, a valid, repeatable solution, able to procrastinate an operation for a long time.
Attention: these are therapies that require the presence of an experienced and qualified professional who develops a therapeutic plan together with an orthopedic specialist in the foot and ankle field.
My personal experience leads me to discourage infiltrative procedures in the ankle. This is absolutely true for cortisones, but recently new forms of viscosupplementation (hyaluronic acids and derivatives), or even intra-articular infiltrations of PRP have been proposed, without a precise scientific rationale. The observed results are mixed and often unstable.
TopNext
Ankle Surgery and Replacement
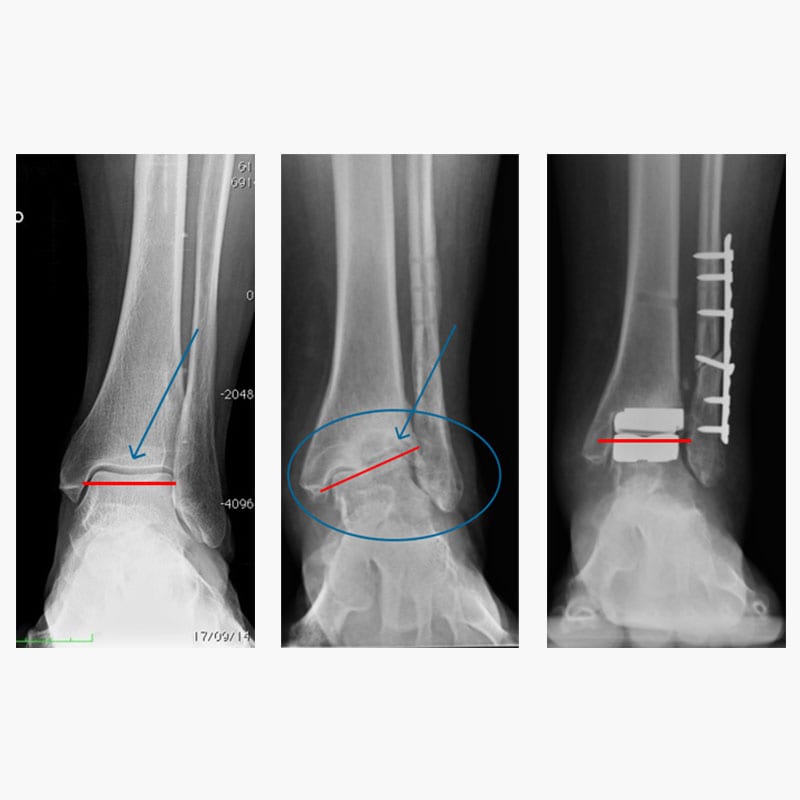
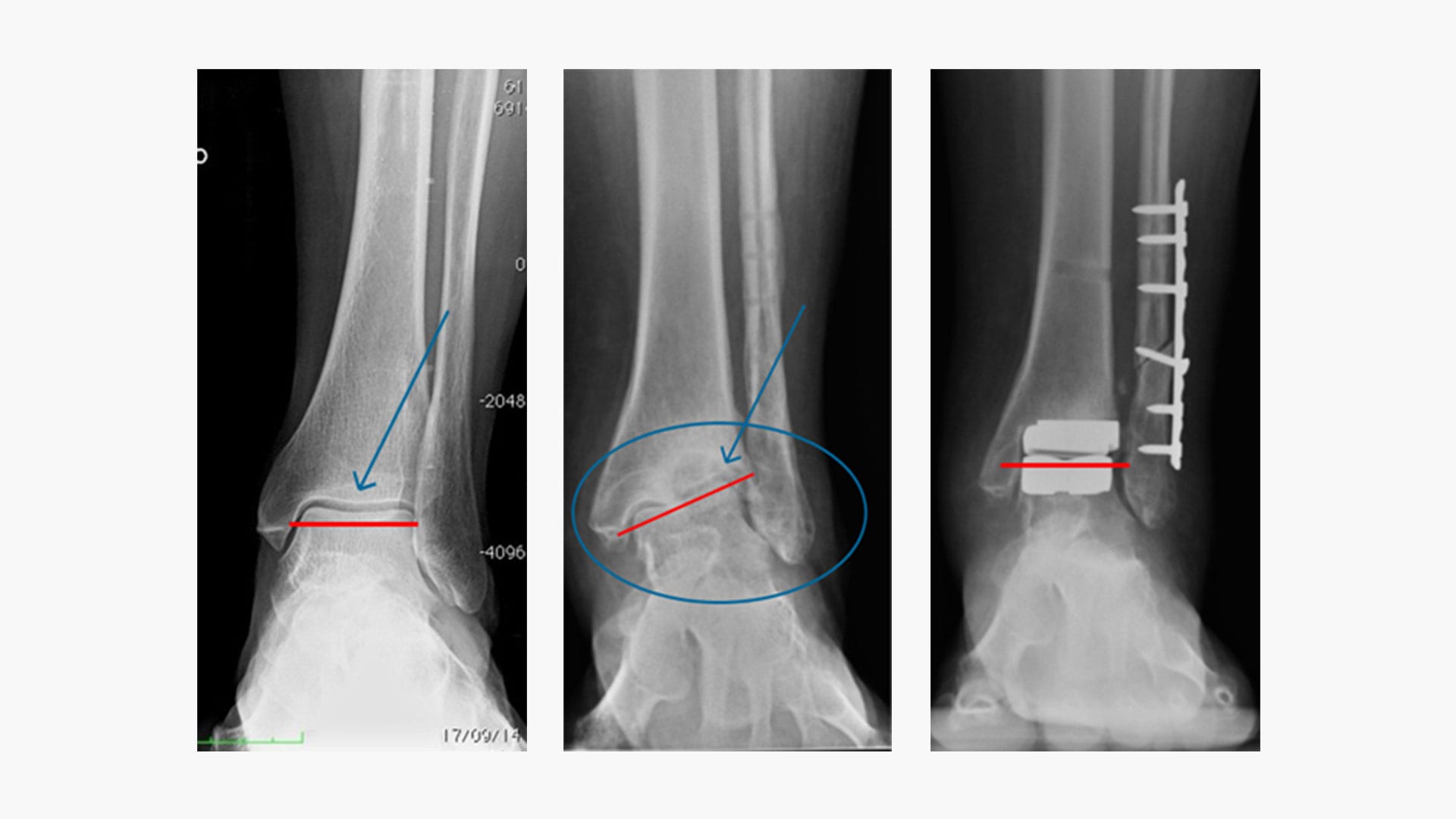
In the three images above we see from left to right: a healthy ankle, a broken ankle, and a prosthetic ankle
There are two different surgical techniques for ankle arthritis: arthrodesis or arthroplasty (replacement).
TopNext
What is Arthrodesis?
Arthrodesis is the fusion of a joint. Below we focus on that of the ankle.
It can be performed either with an incision that exposes the joint or by arthroscopy. In both cases the goal is to obtain a complete fusion of the 90-degree joint.
This implies not only the loss of ankle movement, but also greater stress on the adjacent joints, which will be exposed to a greater workload and, consequently, to a higher osteoarthritic risk.
A young patient undergoing ankle arthrodesis, therefore, runs the risk of developing osteoarthritis in all the other joints of the foot and having to resort to, over the course of life, new procedures of arthrodesis, finding himself with an increasingly rigid foot over time.
TopNext
What is Ankle Arthroplasty?
It is the substitution of the joint with an implant that reproduces the movement and that comes as close as possible to its natural function.
Compared to patients with hip or knee osteoarthritis, those affected by ankle arthritis can be much younger and have greater mobility needs in everyday life. Thanks to the new generation implants, this factor is no longer a contraindication to the replacement.
Even in the case of a pre-existing deformity, replacement can still be used. An essential condition in this case is that the surgeon has a solid experience in ankle prosthetics and reconstruction techniques.
The only contraindication to the replacement is represented by the lack of bone-stock (ascertainable with the CAT scan), meaning the bone reserve on which to support the implant.
Searching for information on the internet regarding prosthetic technique, you can come across a number of opposing opinions to this type of surgery. This wrong school of thought is because of the old prostheses, or replacements, used more than 15 years ago.
Today, we are increasingly moving towards the technique called “resurfacing“, which consists in reducing the volume of prosthetic implants and developing prosthetic designs closer and closer to the original anatomy of the ankle.
This is possible thanks to materials able to reproduce the physical characteristics of the bone, its porosity, stiffness, and elasticity.
For example, the introduction of a material such as Trabecular Metal (Tantalum undergoing a particular process) allows a resurfacing procedure with smaller and anatomical implants, which significantly speed up recovery time. This implant is inserted by a lateral incision, rather than the usual anterior incision.
In Italy I am currently the surgeon who has performed the largest number of surgeries and follow-ups with the technique of resurfacing. It is a revolutionary and reliable choice, which offers great advantages, but which at the moment is reserved for select clinical cases.
Recovery
Prior to surgery, the patient is pre-admitted, during which the patient undergoes blood tests, a further orthopedic check, and an anesthetic evaluation.
The anesthesia practiced is generally of the combined type and is able to remove feeling in the leg for a long time, possibly until the following morning, in order to reduce the use of pain control drugs.
Hospitalization takes place on either the surgery day or the previous day. It can last from 2 to 4 days. Once the surgical wound and pain do not require daily medical checks, the patient will be released.
TopNext
Returning on Field


Ankle replacement surgery is an increasingly frequent procedure that requires a rigorous follow-up and a delicate post-operative course that guarantees immediate osseointegration rather than an early mobilization.
My patients are immobilized with a cast or a brace for 6 weeks, even if putting weight on the foot is generally allowed at 3 weeks.
It is essential that the patient is present at the weekly check-up to complete skin healing (3-5 weeks after surgery).
After 3-6 weeks, the first standing X-rays are scheduled.
Once the plaster or brace is removed walking rehabilitation is essential. For this, I recommend my patients to hydrokinesitherapy (reeducation to walking in the water), stretching triceps, and subsequently proprioceptive rehabilitation.
The patient is self-sufficient about 2 months after the operation, drives a car after 3-4 months, and achieves complete post-operative satisfaction around 6-8 months.
These times are considerably reduced thanks to the new resurfacing procedures which, however, we have to evaluate on a case-by-case basis.
TopNext
Scientific Research and Ankle Arthritis
My commitment to the prevention and improvement of surgery for the treatment of ankle arthritis is shown with daily study and research. To further understand these issues and appreciate my commitment to developing innovations internationally, I invite you to visit the “scientific papers” section.