Ankle Prosthesis
Ankle Prosthesis
Mobile Bearing
Ankle Prosthesis
Resurfacing
From Prosthesis to Prosthesis
Revisions Arthrodesis
From Arthrodesis to Prosthesis
Ankle replacement (or prosthesis) is the solutions for the ankle arthritis.
My Experience


When in 2008, at Duke University, I began to increase my interest of ankle prosthesis, we were still at the beginning of this surgical solution.
In that moment there was talk of isolated experiences; good results in the surgeons’ designs of the implant and mixed results in the rare cases of independent surgeons.
Current solutions were not yet able to be the answer for patients suffering from ankle arthritis since prostheses were still looked at with fear and doubt. The procedure known as ankle arthrodesis was looked at favorably, especially in cases involving young patients and high functional request.
What does arthrodesis mean? It is a surgical procedure that involves the fusion of the ankle in a favorable position to allow the development of a walk by taking advantage of the movement of nearby joints.
It is a solution that we have extensively studied in the past, grasping its weak side, in the alteration of the natural walk and the consequent arthritic degeneration of nearby joints.
TopNext
Ankle Arthritis and Quality of Life
If we were to analyze the characteristics of a patient suffering from ankle arthritis, we would be amazed at what a great negative impact this problem has on their quality of life.
The word “arthritis” is usually associated with advanced age. We imagine an elderly patient, forced to use a stick or two crutches in order to navigate through short distances. We think of a man or a woman for whom it becomes difficult to perform simple daily routines, like putting on a pair of trousers, tying shoes, or getting in and out of a car.
They are patients who oftentimes find themselves forced to abuse analgesics and anti-inflammatories in order to live their daily lives. Due to this approach they risk developing serious problems over time in other organs involved in drug metabolism, such as the liver and stomach.
The above is also true for a patient suffering from ankle arthritis, with an aggravating circumstance; they are generally much younger patients at the height of their social and productive life. For these patients, everyday life becomes a struggle and work often becomes impossible. Depression is a serious threat.
TopNext
Post-Traumatic Ankle Arthritis
The ankle does not become arthritic by old age but, more often than not, following a trauma.
Most of my patients are under 50 years old and have a history of fracture trauma that occurred 5 or 10 years before I met them.
Sometimes the interval between the injury and the development of arthritis is shorter. They are patients, as mentioned, at the height of their lives, who have had accidents:
- riding motorcycles;
- skiing;
- working on a construction site;
- repeated distortion traumas found with ex-soccer players, volleyball players, or basketball players.
Alternatively, it also involves even more unfortunate patients suffering form systematic inflammatory diseases, such as rheumatoid arthritis, systematic lupus eritematosus, or intra-articular hemoglobin deposition diseases, such as hemophilia and hemochromatosis.
They are subjects who often have poor quality bone tissue and serious functional limitations due to the chronic therapies they must undergo.
Mark Glazebrook (a Canadian colleague) in the “orthopedic bible”, the scientific journal “JBJS Am” (2017), recently quantified that the disability of patients suffering from ankle arthritis is superior to the disability caused by knee arthritis and is equal to that of hip arthritis.
This is not a competition for the most misfortunes and diseases, but a way to quantify the serious problems faced by patients with ankle arthritis and to clinically motivate the importance of early and priority treatment.
TopNext
Ankle Fractures and Ligament Injuries
The ankle is an extremely congruent joint, its surfaces match as if it were the most precise of puzzles. It is such a perfect system that, if not compromised, it never gets old.
The ankle is a joint with an intrinsic stability. The role of the ligaments takes over for dynamics or during movement.
Repeated ankle injuries may induce ligament and cartilaginous lesions. The onset of arthritis can be prevented with an early instability treatment, which reconstructs the cartilaginous plane and the injured ligaments.
Fractures can affect the tibia, fibula, malleoli, and talus.
In these cases, an “acute early treatment” aims to restore the original anatomy. It is the first step to prevent osteoarthritis, which could also take place after a satisfying anatomical reconstruction.
An often underestimated role with fractures is seen with the fibula. It is not uncommon to come across patients who have been perfectly operated at the level of the tibial fracture, but in which it was not possible to restore the original length of the fibula. In addition to pain and disability, these patients will develop a valgus deformity in the case of too short a fibula, or a varus deformity in the case of too long a fibula.
Another aspect to be explored is represented by translational deformities. These are deformities in which the talus (the bone of the foot that forms the ankle) becomes unstable and “slides” forward with the tibia relative to its center of rotation. This causes a considerable reduction in the movement of the ankle. Patients suffering from this deformity limp visibly, keeping the limb stiffly on tiptoe and the knee in “recurvatum”.
In these cases, it is important to correct the translational deformity rather than to think of performing “anterior release” with an arthroscopic treatment, which used to be the case. In fact, patients who I see for the first time show significant worsening if they have had an ankle arthroscopy elsewhere.
Arthroscopy is an operation in which, through two mini-incisions, the joint is inspected and cleared. It is a very useful procedure in cartilage lesion cases because it avoids “opening” the joint, thus reducing the risk of post-surgical stiffness.
However, it turns out to be a useless and sometimes counterproductive procedure in cases of impingement and reduction of movement by formations of anterior exostosis.
In these cases, the surgeon’s goal must be to restore the correct axis of rotation of the joint.
This is a very avant-garde concept and is considered a “hot” theme, which my group brought to the forefront of science with our study, recently published in the foot surgery magazine “European Society of Ankle and Foot Surgery “(EFAS).
TopNext
The History of Ankle Arthroplasty: Fix-Bearing and Mobile-Bearing
Ankle prosthesis is a reliable solution for the treatment of ankle arthritis.
The acquisition of today’s excellent results is recent history; in fact, there has been an unstoppable evolution of drawings and tribology (the study of materials and their interaction) over the past twenty-five years. This has come from frenetic scientific activity, which has seen two different schools of thought: American and European.
The Americans produced voluminous prosthetic designs bound to the talus and tibial surfaces. These are prostheses made up of two elements, with a movement linked between the two (Fix-Bearing). Such designs have the advantage of offering a good range of movement of the prosthetic ankle, but the have the disadvantage of being subjected to great mechanical stresses at the level of their interface with the bone. They are prostheses that I got to know in my period of work in the United States and which, frankly, I noted greater long term disadvantages than advantages.
The winning prosthetic concept comes from Europe and is called Mobile-Bearing prosthesis.
In order to reduce the enormous stress that the Fix-Bearing prostheses were subject to, a Danish surgeon (H. Kofoed), was the first to propose a revolutionary three-component design: a tibial component, a component involving the talus, and a mobile polyethylene pad, defined as a meniscus, in order to dissipate the stress of the two main components.
This concept has been greatly popular and has been modified by various authors. The most successful version most likely is the “Hintegra” prosthesis, of which I was one of the main users in Italy, and was designed by Beat Hintermann, who was one of the teachers of my training program and with whom I worked in Switzerland.
The advantages of this prosthesis consisted in the reduced dimensions, therefore, saving the patient’s bone and in an osseointegration that did not require cementation.
The main disadvantage was represented by a discrete rigidity of the system compared to the fix-bearing models.
TopNext
Ankle Arthroplasty Today
Today’s ankle prosthesis is the best standard treatment for symptomatic arthritis of the ankle.
It allows for the patient to maintain a physiological walk without requiring adaptations and consequent overloads to nearby joints. It is compatible with low impact sport activity in younger and more active patients.
It is now clear what the ingredients for a successful replacement are: saving the bone-stock, and the need to obtain an ankle in place at the end of the procedure to guarantee stability and function. All winning prosthetic designs save bone.
This requirement is the prelude to the birth and development of “resurfacing”.
TopNext
Resurfacing Ankle Prosthesis

Resurfacing refers to a prosthesis that has very close characteristics to the natural ankle and which, when implanted, reduces bone sacrifice to a minimum.
In short, resurfacing is a system that allows you to recreate the “shape” of the original ankle, from the preparatory cuts to the insertion of the prosthesis.
It is a very important feature because it allows for a second chance. The more bone the surgeon is able to save, the more the patient will have the opportunity to repair it in the future when the prosthesis has worn out.
Recall that in the ankle case, arthritic patients are younger and more active than patients affected at the hip and knee level. The possibility of being able to provide a revisionary repair is undoubtedly a safety index.
Design is the key to the success of an implant, but it needs to be accompanied by a choice of materials, which amplify the advantages.
Modern prostheses pay great attention to the osseointegration process. It began historically with prostheses coated in “hydroxyapatite” to promote bone metabolism. We have come to what is today defined as the most reliable answer in terms of “integration”: the use of trabecular metal, a metal that is derived from the processing of Tantalum and has very similar characteristics of the bone.
In practice, the bone cells (osteoblasts), “read” it and recognize it as if it were bone itself. They “inhabit” it and perfect its osseointegration without the absolute necessity of resorting to cementation procedures.
TopNext
Ankle Replacement and Learning Curve: The Value of Numbers
Ankle prosthesis is the chosen treatment for ankle arthritis.
An operation burdened, like many others in orthopedics, by an important surgeon “learning curve”. Even the doctor, like any other professional, needs to learn procedure after procedure. This is a crucial aspect for a joint like the ankle, where the general numbers are reduced.
An aspect that my group, as a promoter of prosthetic ankle surgery, has always had at heart, enough so as to publish an interesting article in the journal of European Ankle and Foot Surgery.
We researched the surgeon’s learning curve in about thirty cases of prosthetic ankle surgery. This study reiterates the role of reference centers to ensure a high quality of care for patients suffering from a relatively infrequent pathology, such as ankle arthritis.
These numbers should not be interpreted as solid boundaries, but as an incentive for those who, like us, are involved not only in the care of patients, but also in the training of other colleagues in Europe and around the world.
Today, with over one hundred cases of “Hintegra” prosthesis (Mobile-Bearing prosthesis) and over three hundred cases of TM-Ankle Zimmer-Biomet prosthesis (Fix-Bearing prosthesis or lateral access resurfacing) there is a unique reality in the treatment of ankle osteoarthritis.
The evolution of our choices and our numbers has led us to describe and develop our original surgical technique, which we published in the international scientific journal “Sicot-Journal”.
Today this technique represents a reference in terms of ankle prosthesis with a lateral approach.
TopNext
Our Operating Room
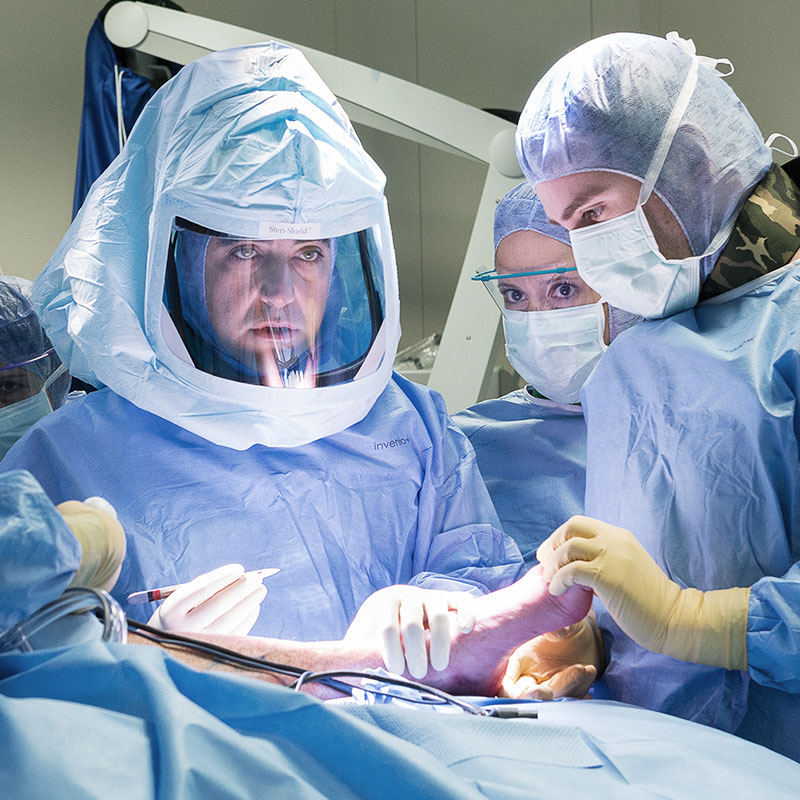
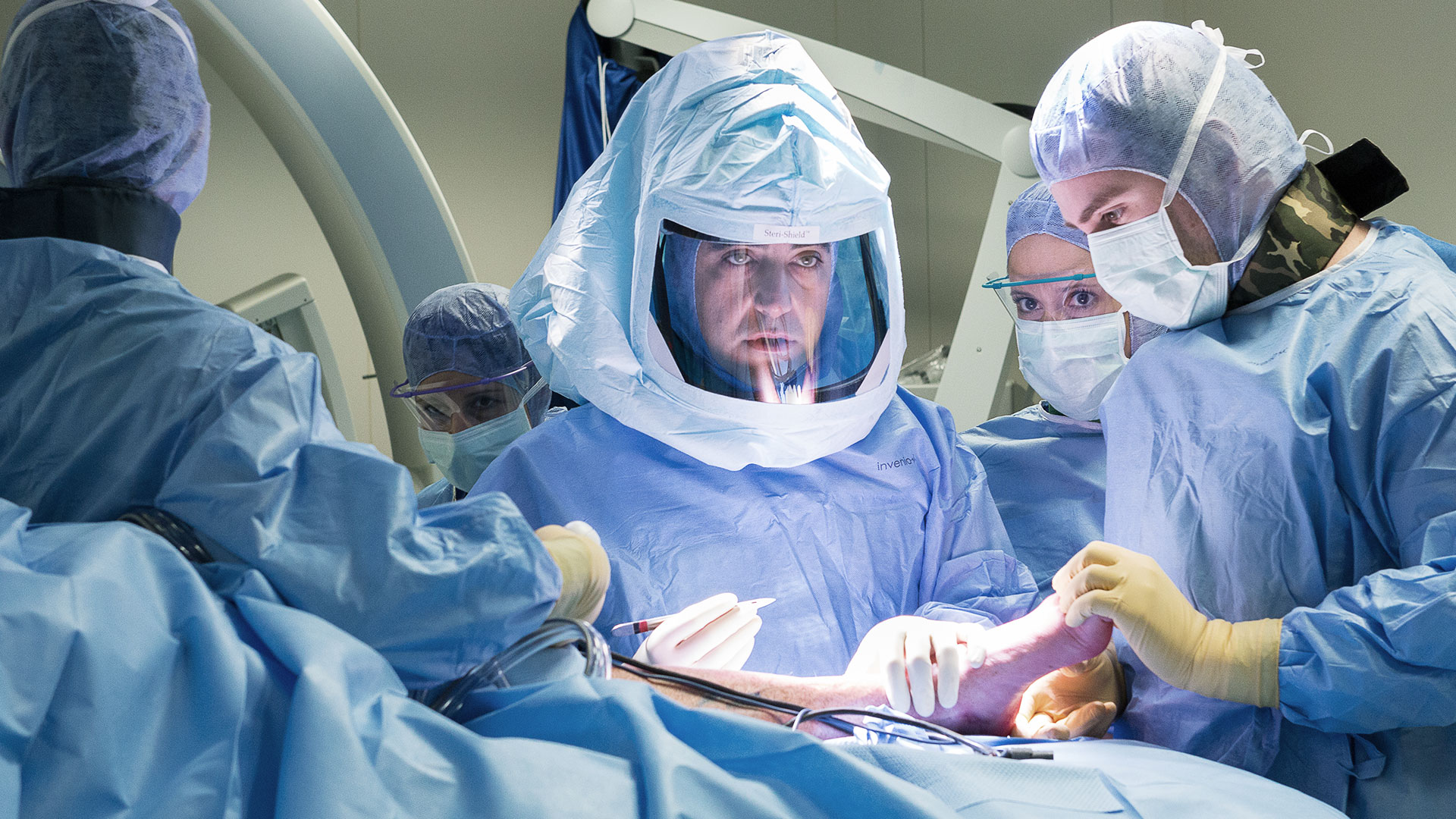
These numbers have allowed for careful evolution of our technique.
I have the privilege of having trained a group of professionals who are an excellence today.
Dr. Indino, Dr. Maccario, and Dr. Manzi are my team, they have grown by my side and today they are much more than trained surgeons. When I see them working and when they are with me I know that they will always be in the right place at the right time. This is a source of great tranquility and serenity, even in the most difficult challenges.
The operating room is not just scalpels and surgeons, it includes organization and technology, where the leap in quality is to make everything reproducible, fluid, and coordinated.
Surgeons who come visit us from all over Europe are often stunned by such an organization. Two operating rooms dedicated to reducing downtime, a recovery room for immediate post-surgery, and a team of dedicated nurses, which are part of the Casco Team. We could not treat so many patients with the same results if we were alone.
When a patient comes to thank me fifty days after surgery, walking on his own, it is the whole team’s result!
TopNext
Ankle Arthroplasty: The Post-Operation Route
After an operation that normally lasts under ninety minutes, the patient is transferred from the operating room to the recovery room, where two nurses and an anesthesiologist worry about immediate post-operation management.
The patient has on a fiberglass boot (ending below the knee), which is put on in the operating room and will accompany him for two weeks. The operated limb will remain anesthetized for a prolonged period, often throughout the night. Blood losses are reduced to a minimum, so blood transfusions are not necessary routine.
The next day, the ankle will be medicated through a lateral opening in the plaster made on the day of the operation.
After two days the majority of patients operated on the ankle have good pain control and can be discharged.
The first check-up is scheduled after fifteen days for the suture removal and plaster removal as well as giving the patient a walking boot, which can be removed at night. This boot will accompany the patient in the recovery program over the next three weeks.
After five weeks from the date of surgery, the patient can place weight on the foot without the boot, and it is possible to abandon the crutches and gradually return to normal habits, including driving.
From this moment, the physiotherapy dedicated to the weight recovery will begin, eventually facilitated by hydrokinesitherapy (walking in water), strengthening, and stretching the triceps.
TopNext
The Value of Teaching


Almost everyday that we operate we receive visitors not only from Italy, but from all over Europe. We have hosted surgeons from France, England, Ireland, Belgium, the Netherlands, Germany, Spain, Poland, Russia and China. They are colleagues interested in the way we treat ankle osteoarthritis.
For the reason that we firmly believe in our work, I felt obliged to accompany these surgeons in their path of approaching arthroplasty by helping them and advising them on their activities.
This often leads me to operating rooms throughout Europe to guide these colleagues as their tutor during their first surgeries. I contributed to the first ankle prosthesis with lateral access in Spain, to the first in Belgium, and to the first revision with a lateral approach in Poland.
In terms of numbers and scientific activity in Europe, we are overturning the paradigm that young Italian surgeons need to go abroad to learn ankle surgery. For this reason, we have developed fellowship and super-specialization courses open to Italian, European, and Asian colleagues, which are having great interest.
Fellowship is a post-specialty training course in which we offer professional training and financial support. This gives young, enthusiastic surgeons the opportunity to be exposed to this surgery, which, in many parts of the world, is still evolving. It gives me, as a professional, the opportunity to be surrounded by enthusiasm, curiosity, and an extra boost in research.
TopNext
Scientific Research and Ankle Replacement: Our Results
When we embraced the concept of the lateral approach, the osteotomy of the fibula, and the new prosthetic resurfacing, it really seemed like a revolution.
The initial reason was to finally have a direct view on ankle’s center of rotation, which remained hidden and inaccessible with an anterior approach.
Today it is the most widespread technique in Italy for many reasons. Most of the acquisitions in this area are linked to our scientific team.
Dr. D’Ambrosi and Dr. De Silvestri daily dedicate their body and soul to the continuous acquisition of data in prosthetics and cartilage reconstruction.
Their activity and our international collaboration have allowed us to achieve unexpected results very rapidly, just as scientific evolution in this area should be: efficient and reactive.
We initially communicated the results of our studies in national and international meetings: SIOT (Italian Society), AOFAS (American Society), and EFAS (European Society).
We later published them in the leading scientific journals of our field: Foot and Ankle International (scientific body of the AOFAS), Foot and Ankle Surgery (scientific body of EFAS).
We believe that the lateral approach allows the surgeon to see and act on one of the most important negative causes or changes that occur in arthritic ankles: the retraction of the posterior soft tissue.
This, in our hands, allows a more effective and stable correction of post-traumatic deformities over time as compared to other techniques.
One of our most relevant studies is the one in which we compared healthy ankles, ankles subjected to a mobile-bearing prosthesis (third generation with anterior approach), and ankles with prostheses with lateral access.
Based on rigorous radiographic analysis, we have shown how the curved cuts and the lateral approach are most effective in restoring an ankle, which is as similar as possible to healthy ankle with remarkable results in terms of movement, a natural walk, and “proprioceptivity” (feeling of the patient having his ankle back again).
Another study that pioneered the treatment of arthritic deformities was the one in which we verified the efficiency and reliability of ankle joint surgery associated with accessory surgical procedures of deformity reconstruction, such as subtalar arthrodesis.
This experience has opened the way for the use of prosthetics even in cases of more complex arthritis, which require surgeries on several skeletal segments to achieve the ultimate goal: an ankle that moves on a leg, and an aligned and stable foot.